Shoulder Instability
The shoulder is comprised of 5 joints or articulations to the body. The primary joint is the glenohumeral joint. This is the ball and socket that allows the arm to be elevated overhead, rotated out to the side or placed behind the back. To allow such large ranges of motion, the joint has a shallow socket which is less constraining. I like to think of the joint as a golf ball sitting on a tee. The shoulder socket (glenoid) is wider than a golf tee but just a shallow. Since the glenoid is part of the scapula (shoulder blade), it is also moving as the ball (humeral head) moves. This makes it more difficult for the humeral head to remain located within the glenoid. Instability commonly results when the ligaments that hold the joint together become damaged or are loose. The glenoid socket is deepened by a cartilage rim that is attached around the perimeter of the socket called the labrum. Damage to the labrum or fractures of the rim of the socket can also make the humeral head more likely to displace out of the glenoid.
Classification of shoulder instability
Shoulder instability is classified by the amount of displacement, the direction of displacement, the frequency of the instability and the overall laxity or looseness of the joint ligaments. A displacement of the humeral head to the edge of the socket without completely coming out of joint is called a subluxation. Complete displacement out of the socket is a dislocation. There are 3 primary directions that the shoulder can sublux or dislocate. The most common direction is to the front or anterior. The humeral head can also displace out the bottom of the socket or inferior. There can also be displacement to the back or posterior. Patients with ligament laxity (especially if "double-jointed") will have instability in all directions called multidirectional instability. A common test for ligament laxity is the ability to pull the thumb back to touch the forearm just above the wrist. Hyperextension or back-bending of the elbow and knee are also signs of joint laxity. A shoulder that has subluxed or dislocated more than once has recurrent instability.
Traumatic instability
A fall on the outstretched arm or a sudden jerk of the arm behind the body can cause the humeral head to dislocate out of the glenoid. The dislocation usually requires someone pulling on the arm to reduce it. There is frequently a tear of the labrum or damage to the ligaments that support the joint. A tear of the labrum in the front and bottom corner of the socket is referred to as a Bankart lesion. A similar tear can occur in the back of the glenoid with a posterior dislocation and is called a reverse Bankart lesion. Occasionally, a small piece of articular cartilage covering the glenoid will also tear with the labrum (GLAD lesion). A small piece of bone may also fracture as the humeral head dislocates (bony Bankart). The ligaments in the front of the shoulder can be torn away from their attachment on the glenoid (ALPSA lesion) or from their attachment on the humeral head (HAGL lesion). Correctly identifying the type of tear is important to determine the correct treatment.
Atraumatic instability
Instability that occurs from minor trauma is referred to as being atraumatic. The shoulder can sublux or dislocate just with reaching in an awkward position in people with ligament laxity. There is usually nothing torn and MRIs are frequently normal in this setting. Recurrent instability is common and the joint is usually self reduced. Patients often have a history of joint laxity and the instability is often not as painful. Some patients can actually sublux or dislocate their shoulder voluntarily. On physical exam, the instability is usually multidirectional.
Treatment of traumatic instability
The treatment of a tear of the labrum or capsule is dependent upon the patient's age, activity level and severity of the tear. Many studies have documented a 75-90% recurrence rate for a shoulder dislocation in young adults less than 25 years of age who have a traumatic dislocation and Bankart tear. There is also a greater risk if the injury is to the dominant shoulder in a person who participates in contact sports. I will counsel the patient regarding this risk. Many patients opt for immediate surgical repair to avoid a recurrence of the severe pain they experienced with the shoulder dislocation. The risk of recurrent dislocation after an arthroscopic Bankart tear repair is now less than 10% with modern techniques. Patients over 40 years of age have only a 10% risk of recurrent instability without surgery. After initial immobilization in a sling, physical therapy to strengthen the shoulder will often allow them to avoid surgical repair. For patients in the middle age range (between 25 and 40 years of age) the risk of recurrent instability is approximately 50%. Their treatment will often depend upon their activity level. Those who are not involved in contact sports can often be managed nonoperatively. When considering surgical repair for shoulder instability, it is important that the surgeon has significant experience in treating these tears. An arthroscopic repair can be a technically demanding procedure and requires that the repair is secure, anatomic (without over tightening the joint) and that all other instability factors such as ligament laxity are addressed. This will significantly reduce the recurrence rate after surgery.
Arthroscopic image of a Bankart tear. The gold probe
is lifting the torn labrum away from the white colored
glenoid cartilage.
Arthroscopic repair of the torn Bankart lesion.
Anchors (not seen) have been inserted into the bone
at the tear location. Sutures (aqua colored) are passed
around the torn labrum and arthroscopically tied.
Treatment of atraumatic instability
The great majority of patients with atraumatic instability can be managed without surgery. There is usually nothing torn that would require repair. Many patients with atraumatic instability present with shoulder pain rather than a feeling of the shoulder being unstable. They have never experienced a dislocation or noticed a subluxation. The pain originates from the rotator cuff which is the primary dynamic shoulder stabilizer. When the shoulder joint is loose, the rotator cuff helps stabilize the joint. This can lead to an overuse inflammation of the tendons. Flexibility of the shoulder is beneficial for many sports but can place additional strain on the rotator cuff.
Strengthening of the surrounding muscles (primarily the rotator cuff) will help dynamically stabilize the shoulder joint. Stabilization of the scapula is also helpful. Physical therapy is of great benefit but it will require continued maintenance of shoulder strengthening exercises for months. Activity modification is also necessary for instability in athletes. Some overhead activities that place the arm behind the body may need to be avoided until the shoulder is stronger. A swimmer, for example, may have to eliminate butterfly and freestyle until the pain is improved. A baseball pitcher may have to reduce throwing until they can do so comfortably. Continuing to stress the shoulder while it is painful will only create further inflammation and pain.
Occasionally, despite months of therapy and activity modification, the shoulder continues to remain symptomatic. In these instances, surgical stabilization may be necessary. The shoulder capsule and ligaments can be arthroscopically tightened by making small tucks in the ligaments and capsule with sutures. Appropriately tensioning the ligaments can restore better joint stability and reduce the strain on the rotator cuff tendons. This will improve pain and allow many to return to their previous sport's participation.
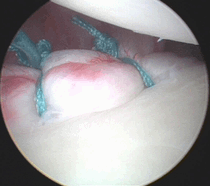
Shoulder plication. Note the fold in the capsule.
The green sutures also pass around the labrum
prior to being tied
Key Points to Treating Shoulder Instability
1. First determine if the instability is due to a traumatic tear or ligament laxity
2. Tears of the anterior labrum (Bankart tears) have a high likely of recurrent instability in young, athletic males.
3. Tears in older patients (over 40) can usually be managed without surgery.
4. Strengthening the rotator cuff and scapula stabilizing muscles helps stabilize the shoulder joint.
5. Arthroscopic repairs in the hands of experienced shoulder surgeons (such as Dr. Payne) have success rates that equal or surpass the historical success rates of open surgery.